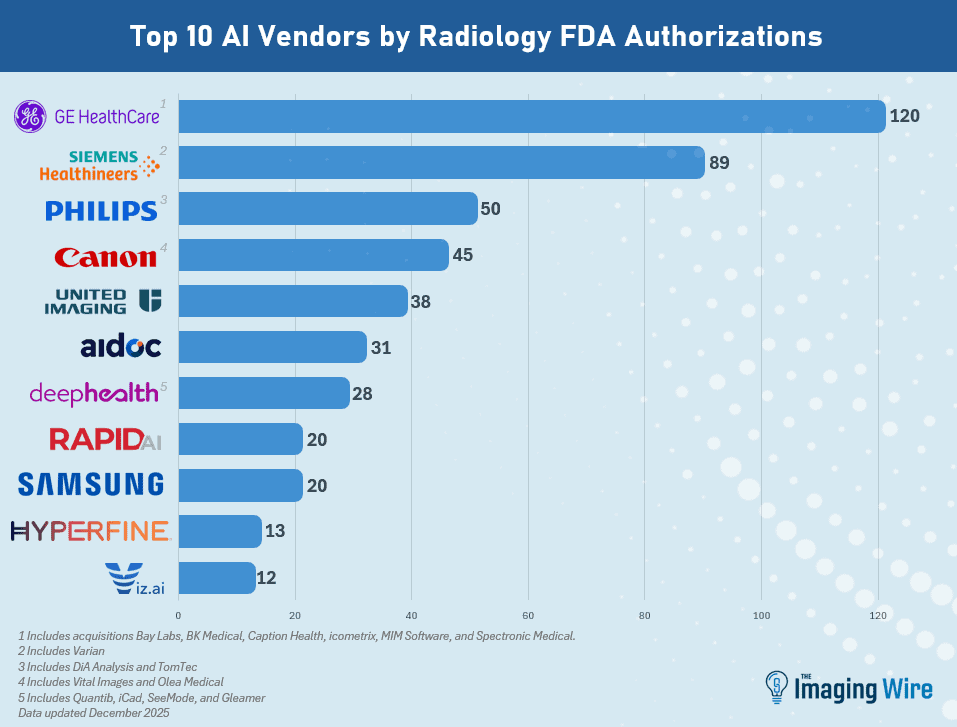
Momentum is building toward routine clinical use of AI for breast cancer screening. Several new studies offer even more support for mammography AI, including research published today in Nature Medicine in which AI reduced radiologist workload by over 60% by excluding low-risk studies from human review.
Breast screening has become one of the most promising use cases for AI, with the potential to reduce radiologists’ workload while improving their ability to detect cancer.
- For example, the recent MASAI study found that ScreenPoint Medical’s Transpara AI algorithm could replace the second human reader in a double-reading protocol, reducing workload by 44% and improving cancer detection rates by 28%.
The new research in Nature Medicine also used Transpara, as part of the AITIC study in Spain with the goal of seeing if AI could triage low-risk studies so they don’t require review by human radiologists.
- AITIC had a prospective design, involving 31k women with screening exams split between 2D mammography (17k) and digital breast tomosynthesis (14k).
Women in the control arm of the study got conventional double reading by two radiologists – the standard mammography paradigm in Europe.
- The intervention arm used a partially autonomous AI approach: cases that AI interpreted as low risk were classified as normal and were not reviewed by radiologists, while all other cases were double-read by radiologists using AI support.
In analyzing the results, researchers found…
- Workload in the AI arm was 64% lower than conventional double reading.
- AI’s workload reduction was similar between DBT and conventional digital mammography (-66% and -62%, respectively).
- The AI arm’s cancer detection rate per 1k women was 15% higher (7.3 vs. 6.3 cancers).
- But the recall rate was also 15% higher.
It’s worth noting that the AITIC study differed from MASAI in its inclusion of DBT screening exams, whereas MASAI only included 2D digital mammography.
- While 2D mammography is the norm in Europe, much of the U.S. has switched to DBT for breast screening, so the AITIC results offer good news for U.S. breast imaging practices considering AI adoption.
The Takeaway
The AITIC study’s new results are powerful confirmation of findings from the recent MASAI trial and support broader clinical deployment of mammography AI. Taken together with positive findings from last week’s Nature Cancer articles (see The Wire section in this newsletter), they paint a picture of a technology that’s ready for prime time.