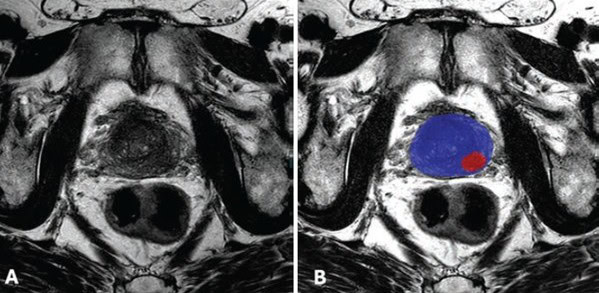
Routine prostate cancer screening currently isn’t supported by clinical guidelines. But that could be changing, especially given research presented this week finding that prostate screening – aided by MRI to reduce unnecessary biopsies – was as effective as mammography screening.
Prostate cancer is one of the leading causes of cancer death, killing some 360k men worldwide every year.
- But efforts to develop effective prostate cancer screening programs have been hampered by the challenges inherent in PSA testing, which often identifies indolent disease that may never pose a health risk to patients – the classic definition of overdiagnosis.
That could be starting to change, however. Researchers are discovering that using MRI to work up patients with rising PSA levels could help identify men with high-risk disease who should be sent to biopsy, while lower-risk patients are monitored with surveillance.
- New research presented at the European Association of Urology meeting on Sunday supports this idea, showing that – if done right – prostate cancer screening can be as effective as mammography screening.
Researchers from Germany compared prostate cancer screening data from 39.4k men who got PSA tests as part of the PROBASE trial to over 2.8M women who participated in the country’s national breast cancer screening program.
- Under the PROBASE protocol, men with confirmed PSA levels ≥ 3 ng/mL underwent MRI and biopsy, while those with lower PSA levels got repeat PSA testing in an effort to keep biopsy rates lower.
Major findings of the study included…
- Both breast and prostate screening detected a high rate of clinically significant, invasive cancers (73% for mammography vs. 69% for 45-year-old men and 74% for 50-year-old men).
- False-positive rates were much lower for breast screening (10% vs. 42% and 37%).
- And fewer indolent cancers were detected with mammography (22% vs. 31% and 26%).
- But biopsy rates were comparable (1.1% vs. 0.8% and 2.4%), as the study’s active surveillance protocol limited over-treatment.
While the PROBASE study didn’t use AI as part of its protocol, other research has found that AI analysis of MRI scans can make the modality even more precise, with the PI-CAI study just one worth noting.
The Takeaway
Is it finally time for prostate cancer screening to join breast, colorectal, cervical, and lung among the major population-based cancer screening tests? Results from the PROBASE study at EAU 2026 suggest the time may finally be right.